Contact us
Our team would love to hear from you.
Errors remain common in clinical coding because documentation is often incomplete or inconsistent, coding rules are complex, and teams face staffing and time pressure. The healthcare industry loses approximately $23–38 billion annually due to documentation problems, including coding errors. Yet few providers use AI to mitigate downstream denials, only 14% of U.S. providers reported doing so in 2025. Expanding well-governed automation and AI can significantly improve coding, increasing its accuracy and speed and reducing denial-related revenue loss. Moreover, automation of routine, high-volume tasks allows human coders to focus on complex cases that require clinical judgment.
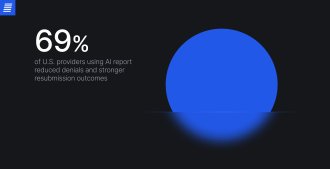

Source: experianplc.com
There are several cases where AI makes coding smarter and more reliable.
AI is more than technology—it’s a game-changer for coding solutions. Here’s how it influences the entire RCM.

“AI-driven clinical coding brings a level of precision that traditional methods simply can’t match. By automating repetitive tasks, AI reduces errors and administrative workload, allowing teams to focus on what matters most: quality patient care.”
Healthcare Solutions Consultant
How does AI in clinical coding work? AI subsets and complementary technologies perform different functions in this process to achieve efficiency and accuracy.
Natural language processing (NLP) algorithms are used to understand and interpret human language, enabling machines to process and analyze unstructured medical records (such as clinical notes). NLP extracts relevant information (e.g., diagnoses, procedures, and medications) and maps it to standardized codes, such as ICD-10 and CPT codes.
Machine learning (ML) algorithms identify coding patterns in historical data to predict and verify the most appropriate codes, while generative AI (GenAI) can interpret unstructured clinical notes and suggest relevant codes. These technologies reduce human error, streamline the coding process, detect fraud in billing and claims data, and predict denials, helping healthcare organizations handle them in advance.
Computer vision algorithms process scanned medical records, extracting text from image-based medical documents and converting it into machine-readable text. Once digitized, the text can be processed by NLP algorithms for further analysis, making even non-digital medical records part of the digital coding workflow.
Robotic process automation (RPA) enhances automation capabilities by reducing the need for manual data entry and handling rule-based coding tasks. RPA bots ensure that all required fields are filled before submission, reducing errors and denials. RPA in medical billing and coding functions as the “hands” of automation, performing consistent and repetitive tasks without human intervention. Unlike traditional manual coding, automated processes with RPA speed up workflows and reduce the potential for human error.
| Traditional medical coding | Automated medical coding | |
|---|---|---|
| Process | Manual coding, which is labor-intensive | Coding assistance, suggestions, etc. |
| Speed | Slow process that depends on human effort | Fast process enabled by automating manual tasks |
| Accuracy | Variable, error-prone | High accuracy and consistency, improves with learning |
| Cost | High staffing and operational costs | Low long-term costs, though setup costs can be high |
| Scalability | Limited | Easily scalable |
| Compliance | Prone to compliance issues due to manual updates and guideline misinterpretation | Easy to maintain compliance with built-in rules and automated update checks |
| Best at | Handling complex tasks | Large-scale routine coding and sophisticated coding tasks |
We developed high-performance, modern, and intuitive Power BI dashboards that improved financial reporting and enabled faster decision-making.
Before integrating AI into the medical billing and coding processes, it’s important to understand the complexities that come with it and be prepared to tackle them. Following are some of the most common challenges of AI implementation.
The use of AI in healthcare is subject to specific laws and compliance requirements, such as the EU AI Act, GDPR, HIPAA, and the HITECH Act, which ensure patient safety, data privacy, and ethical feasibility. Having a comprehensive checklist for medical coding software and adherence to best practices can help avoid any legal issues and ensure AI healthcare compliance.
In the healthcare industry, data is unstructured and usually scattered across different systems, such as electronic health records (EHRs) and billing, leading to incorrect or missing codes. Data preprocessing, standardization, and cleaning can mitigate this issue, with human-in-the-loop and continuous AI model monitoring increasing the quality of outputs. Documentation should include treatment plans and imaging status (performed or ordered) so key clinical details aren’t missed.
AI systems in clinical coding often struggle with accuracy when handling rare or highly complex cases. If unusual diagnoses or procedures are underrepresented in historical data, the system has limited exposure to them, leading to inaccurate coding suggestions. Ensuring accuracy requires large, high-quality datasets and continuous updates.
Many healthcare organizations still rely on legacy systems that lack the capabilities necessary for smooth AI integration. This process can also interrupt established workflows if implemented carelessly. By working closely with a skilled AI team, healthcare organizations can overcome interoperability issues, achieve seamless workflow alignment, and meet their unique needs.
Each medical specialty uses different coding sets, with some more complex and detailed than others. Documenting a patient encounter also varies greatly across specialties and providers. To ensure accurate coding across specialties, clinical coding systems need specialty-specific NLP models, with training/fine-tuning and workflows tailored to each specialty’s documentation.

We’re proud to share that EffectiveSoft has been recognized as one of the key players in agentic AI. This recognition comes from the global report “Agentic AI in Digital Engineering Market 2025-2029” by Reserch & Markets, where we are listed alongside NVIDIA, OpenAI, Google Cloud, and Accenture.
by Research & Markets
As an AI medical coding software development company with over 19 years of experience in healthcare technology, we understand the challenges medical organizations face, and tailor our approach to each client’s needs. Here’s an overview of our process:
Our team conducts a thorough analysis of your current architecture and datasets, identifying gaps and inconsistencies that must be addressed to ensure seamless integration.
We collect, clean, and preprocess data for further use. This is an essential step because AI systems depend on high-quality clinical data.
Before committing to development, we verify system feasibility by designing mock-ups, proof-of-concept models, and prototypes. Our team ensures a user-friendly interface and intuitive navigation.
Our team selects specific algorithms based on project requirements and architecture design. We implement business logic and establish required data flows and system integrations, while ensuring compliance with data privacy standards.
Once the system is developed, our team performs unit and integration testing to evaluate accuracy, consistency, and reliability.
Upon comprehensive testing, we roll out the software in phases and integrate it with existing systems, such as EHRs, and workflows. This step involves training and onboarding end users if necessary.
Our AI-based medical coding services include post-launch maintenance and support. We monitor model performance and compliance and continuously improve it, updating the system to align with evolving standards and requirements.
While the use of AI is gaining traction across the revenue cycle, including medical coding automation, this technology is not designed to replace coding specialists. It is intended to augment their work. Implementing AI gives healthcare organizations the boost they’ve long required, streamlining clinical coding and medical billing automation, reducing the chances of claim denials, and improving cash flow. The experts at EffectiveSoft will help you explore the potential of AI in medical billing and coding and how to integrate it into your processes. Reach out to us to learn more and start your project.

AI healthcare coding software refers to application software that uses AI to automatically convert clinical documentation into standardized codes used for insurance claims, billing, and other purposes.
Applying NLP algorithms, AI identifies key clinical entities, such as diagnoses, procedures, symptoms, and medications, in medical data (usually unstructured). Then, AI models extract relevant medical terms and map them to standard codes, including ICD-10 and CPT. Software checks payer and regulatory rules and validates the results, which are then entered into the billing system. Including a human-in-the-loop approach can help refine the system through continuous learning based on feedback.
AI-enabled coding software can and often does integrate with EHR and other practice management systems in place. Leveraging standards like FHIR, EffectiveSoft engineers design revenue cycle management AI solutions that fit effortlessly into existing workflows, enhancing accuracy and efficiency and reducing administrative burden.
Different types of healthcare organizations can benefit from AI medical billing and coding software. This technology delivers the greatest value to companies with high claim volume and complex structure, such as large health systems and hospitals, multispecialty clinics, RCM companies, specialty practices with complex coding (oncology, cardiology, etc.), and healthcare practices with staffing shortages.
The accuracy of AI systems compared to human coders depends on several factors, including the type of AI system, training data, and clinical domain. AI’s key strengths are speed, scalability, and consistency, but it struggles with contextual judgment. So, while AI is effective in high-volume routine coding, human assistance is necessary for complex or rare cases.
The use of artificial intelligence medical billing and coding software requires strict adherence to industry regulations, which depends on how the software is built, deployed, and used. At EffectiveSoft, we maintain compliance with HIPAA, GDPR, and other regulations through a multilevel strategy that involves implementing strict access controls, data encryption and anonymization, detailed logging, and other best practices to enable security at each step and safeguard sensitive information.
The cost of AI-powered coding software depends on several factors, including project complexity, compliance needs, integrations, infrastructure needs, team size, and development time. Contact our team for a customized project estimate based on your specific requirements.
The integration timeline varies depending on various factors, such as implementation approach, compatibility with the existing management system, and specialty-specific coding requirements. Let’s discuss your project so we can create a realistic timeline for you.
AI is transforming healthcare coding, with AI medical coding companies at the forefront of this change. Hyperautomation can orchestrate entire billing workflows across the revenue cycle while delivering advanced analytics for deeper insights. Because AI processes vast amounts of data and identifies patterns faster than humans, it can significantly improve coding accuracy and help providers better compete for quality reimbursement by ensuring codes are captured correctly.
Can’t find the answer you are looking for?
Contact us and we will get in touch with you shortly.
Our team would love to hear from you.
Fill out the form, and we’ve got you covered.
What happens next?
San Diego, California
4445 Eastgate Mall, Suite 200
92121, 1-800-288-9659
San Francisco, California
50 California St #1500
94111, 1-800-288-9659
Pittsburgh, Pennsylvania
One Oxford Centre, 500 Grant St Suite 2900
15219, 1-800-288-9659
Durham, North Carolina
RTP Meridian, 2530 Meridian Pkwy Suite 300
27713, 1-800-288-9659
San Jose, Costa Rica
C. 118B, Trejos Montealegre
10203, 1-800-288-9659