Contact us
Our team would love to hear from you.
Managing healthcare claims remains one of the most intricate and costly administrative functions. Manual processing increases errors, leading to incorrect payments, rework, and customer attrition. A 2025 survey found that 41% of providers reported denial rates of 10% or higher, highlighting persistent rework and payment friction in claims processing. Administrative overhead accounts for about 25% of total U.S. healthcare spending, underscoring the scale of non-clinical cost in the system.
These figures reflect more than just financial strain—they highlight deep-seated inefficiencies. Manual workflows, data inaccuracies, outdated coding, and time-consuming denial management in medical billing all contribute to delayed reimbursements, stale cash flow, and frustrated staff and patients.
This difficult reality creates an opportunity for AI. Through intelligent document processing, automated coding, and fraud detection, AI can overhaul claim operations—speeding processing, raising first-pass acceptance rates, strengthening compliance, reducing fraud, and improving transparency for patients. Among the minority of providers already using AI, 69% report fewer denials and/or improved resubmission success. The result is a smarter, more reliable claims ecosystem for payers, providers, and patients.
Let’s map the modern claim management workflow:
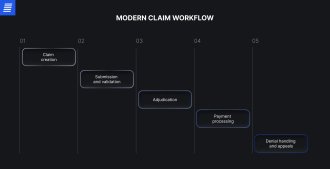

Despite being labeled “modern” and driven by digital tools, this process is still riddled with friction:
To put this into perspective: nearly $25 billion is spent each year on claim processing inefficiencies. In 2024, about 11.8% of claims faced initial denials, up from 11.5% the previous year.
This blend of human error, outdated workflows, system complexity, and increasing compliance demands makes claim management not only one of the most vulnerable and costly administrative functions but also the most urgent target for intelligent transformation.
Historically, healthcare claim management relied on a patchwork of manual reviews, static business rules, and disjointed systems. AI is fundamentally changing this outdated routine. From data capture to denial resolution, AI tools are not only streamlining processes but also making them smarter, faster, and significantly more reliable. Below, we break down where these capabilities are making the biggest impact.
Claim management begins with a lot of paperwork. AI-powered optical character recognition (OCR), combined with natural language processing (NLP), now allows systems to automatically extract relevant information from scanned medical records, electronic health record (EHR) notes, insurance forms, and explanation of benefits (EOB) documents. IDP accelerates claim initiation and improves data accuracy, eliminating manual data entry and reducing transcription errors. Providers have reported noticeable reductions in claim preparation time, frequently described as double-digit percentage improvements.
One of the most prevalent and costly factors behind claim denials is coding errors. AI-driven coding assistants analyze clinical documentation in real time, suggesting appropriate ICD-10, CPT, and DRG codes based on the content of physician notes, diagnostic reports, and operative summaries. These tools reduce the burden on human coders and minimize miscoding incidents, leading to higher first-pass acceptance rates and lower rework volumes. In some healthcare systems, AI-assisted coding has cut denial rates related to coding mistakes by nearly 30%.


Source: healthcarereaders.com
Before a claim is even submitted, AI-powered predictive models help providers understand how it is likely to be received. Trained on historical claims data, these algorithms can forecast approval probability, expected processing times, and denial likelihood with remarkable accuracy. By flagging high-risk claims early, providers can correct documentation errors, validate codes, or gather missing information to address potential problems in advance. For instance, if a high-value procedure such as a major orthopedic surgery shows a strong likelihood of denial based on historical data, staff can proactively ensure that preauthorization and all necessary documents are completed before submission.
Even with proactive measures in place, claim denials remain a stubborn and costly part of the revenue cycle management (RCM) process. AI is changing the approach organizations respond from manual rework to targeted, data-driven action. A key strength here is automated root-cause analysis: as soon as a claim is denied, AI pinpoints the underlying issue, whether it’s documentation gaps, coding mismatches, or eligibility errors, and suggests specific corrective actions. More advanced models also predict the likelihood of a successful appeal, allowing teams to prioritize high-value, recoverable denials and avoid chasing low-probability cases.
The claims process doesn’t end with adjudication. Providers and patients often need updates, explanations, or assistance in resolving disputes. AI enhances this post-claim experience with conversational tools like chatbots and voice assistants, as well as backend systems that provide real-time claim status alerts, document requests, and explanation of benefits (EOB) support. For providers, this means faster access to the information they need and fewer administrative bottlenecks. For patients, AI handles frequent coverage and billing questions. This reduces the burden on call centers and improves transparency.
Healthcare billing fraud happens in many forms, including billing for services not rendered, unbundling, and upcoding. Traditional detection methods rely on rule-based checks and manual audits, which often fail to catch subtle patterns and don’t scale well. AI changes the way this problem is approached by shifting fraud detection from reactive control to proactive, adaptive intelligence. By learning continuously from massive, complex datasets, AI can identify hidden relationships, detect anomalies that static rules may overlook, predict potentially fraudulent activity before payment, and uncover new fraud patterns as they emerge.
Omega Healthcare, a leading medical revenue cycle management provider with over 30,000 employees and nearly 250 million annual transactions, needed a more scalable solution to handle growing volumes of clinical documentation. To address this, the company adopted UiPath’s AI-driven Document Understanding platform, featuring OCR and NLP to extract and organize data from disparate healthcare documents. Here are the key outcomes:
A top-tier U.S. insurer serving over 3 million members integrated Appian’s low-code platform with AI technologies provided by Brillio to modernize its claim adjudication process. Prior systems were hindered by fragmented workflows and time-consuming manual reviews. The solution combined OCR, intelligent form processing, sentiment analysis, and machine learning (ML) models to triage and prioritize claims based on predicted outcomes. Here’s what they achieved:
In an effort to combat rising fraud and waste, Personify Health partnered with Health at Scale, the Massachusetts Institute of Technology (MIT), and the University of Michigan to deploy an advanced, real-time claims screening platform. The system was designed to detect irregular billing patterns and provider behavior. It could analyze vast datasets across regions, services, and time frames with high precision, flagging problematic claims before payment. The results are as follows:
Integrating AI with legacy systems is challenging because many healthcare organizations and insurers rely on outdated infrastructure. This increases implementation costs, slows deployment timelines, and limits the full potential of AI-driven claims automation.
The lack of transparency in complex AI models can increase the risks of litigation, regulatory scrutiny, and compliance concerns, especially when organizations can’t clearly explain how an AI system reached a decision. AI can also create uncertainty about legal responsibility when errors occur. Strong governance, HIPAA/GDPR compliance, explainability, and auditability are essential.
AI trained on historical claims and billing data may replicate human biases and systemic disparities. If not addressed, AI systems may unintentionally reproduce or amplify inequities when evaluating claims, potentially leading to discriminatory outcomes for certain providers, patient groups, or medical services.
Fully automated medical claims processing remains difficult for complex or unique cases. Even with claims automation in place, human intervention is often necessary because claims data can be highly complex, variable, and sometimes incomplete, and because many coverage and payment decisions depend on clinical and administrative context that is not always reliably captured in structured fields.
We developed a management system for enhanced medical billing and insurance claim submission and processing.
To get the most from AI in medical claims management, healthcare organizations can follow proven best practices.
AI is already changing claim management, and the next wave of innovation will bring these tools even deeper into healthcare operations. Here are the key trends to watch.
As the healthcare system shifts away from fee-for-service toward value-based reimbursement models, AI will play a key role in aligning claims data with clinical outcomes and contract terms. You can expect to see AI-driven adjudication tools that factor in quality metrics, risk scores, and bundled payment conditions, ensuring claims reflect not just services rendered, but value delivered.
Training healthcare AI models is heavily constrained by data privacy concerns. Federated learning is emerging as a way to build smarter AI models while protecting sensitive patient information. This approach could help payers, providers, and AI vendors improve claim prediction and denial management while remaining compliant with HIPAA or other privacy regulations.
Instead of reacting to denials and payment delays, future RCM strategies will leverage AI to proactively flag potential claim issues before submission. These systems will assess claim completeness, coding accuracy, and payer-specific risks in real time, increasing initial acceptance rates and reducing downstream financial headaches.
Contract negotiation between payers and providers has traditionally been a complex, manual process. AI is poised to change this space for good, with tools that can analyze historical claims data, forecast the financial impact of proposed contract terms, and identify negotiation opportunities, giving healthcare organizations more control over reimbursement rates and operational risk exposure.
Today, it’s clear that AI is no longer a fringe experiment in healthcare claim management but a proven tool delivering a real operational advantage. From reducing processing times and denials to catching fraud to improving billing transparency, AI provides tangible results at every stage of the revenue cycle.
For health systems and insurers facing rising costs, staffing shortages, and intensifying patient expectations, adopting AI-driven solutions isn’t optional—it’s essential for operational stability and competitive relevance. The organizations leading this charge aren’t just optimizing claims—they are helping build a healthcare system that is smarter, faster, and fairer.
Ready to bring AI into your claims process? Contact our team to start building the right solution for your organization.

AI in claim processing and management involves using AI technologies like ML and NLP to automate and improve efficiency and accuracy.
Some of the key benefits of implementing AI in RCM include streamlined claim processing, improved accuracy, reduced costs, better decision-making, and enhanced customer experience. AI and ML can analyze data to forecast claim volume by provider, region, or season and predict claim complexity and costs, allowing teams to estimate reimbursement amounts, anticipate denial risk and optimize staffing based on expected workload. AI can also help detect and prevent fraud through pattern recognition and real-time alerts and protect data by identifying anomalies in data patterns and preventing cyberattacks.
Healthcare systems like RCM handle a vast amount of sensitive data, referred to as protected health information (PHI), which should remain protected and secure. When implementing AI-powered RCM, companies should follow industry standards, regulations, and best practices for encryption, secure data storage, strict access controls, data anonymization, continuous monitoring and auditing, and compliance frameworks.
While AI has the potential to significantly improve claim processing, it also comes with risks and limitations, including potential bias or inaccuracies stemming from training data, lack of transparency, regulatory and compliance concerns, and difficulties integrating AI with legacy systems.
AI speeds up and simplifies medical claim management by automating routine tasks and intelligently routing claims based on complexity, sending straightforward cases for faster processing while escalating complex ones to specialists. Using machine learning on large volumes of historical claims data, it can also forecast likely claim costs, detect potential fraud, and flag suspicious submissions for human review.
AI tools usually connect to EHRs through standard healthcare interfaces like FHIR APIs or HL7 feeds, often via an integration engine that maps the EHR data into a claims-ready format. They pull the key details needed for billing (diagnoses, procedures, clinical notes, encounter information) to check documentation completeness, support coding, and flag denial risks. The AI then sends alerts or tasks to the billing team’s workflow system. Access is controlled with HIPAA safeguards like role-based permissions, encryption, and audit logs.
A typical implementation could run 8-24 weeks to develop a working pilot, and 3-6 months to reach a stable production rollout (for a simple system). However, timelines depend heavily on integration complexity, data quality, security/compliance reviews, and other factors. Contact our team to get a tailored estimate for your project.
Can’t find the answer you are looking for?
Contact us and we will get in touch with you shortly.
Our team would love to hear from you.
Fill out the form, and we’ve got you covered.
What happens next?
San Diego, California
4445 Eastgate Mall, Suite 200
92121, 1-800-288-9659
San Francisco, California
50 California St #1500
94111, 1-800-288-9659
Pittsburgh, Pennsylvania
One Oxford Centre, 500 Grant St Suite 2900
15219, 1-800-288-9659
Durham, North Carolina
RTP Meridian, 2530 Meridian Pkwy Suite 300
27713, 1-800-288-9659
San Jose, Costa Rica
C. 118B, Trejos Montealegre
10203, 1-800-288-9659